Clinical Study of Battlefield Acupuncture for Acute Pain and Edema Management in Distal Radius Fractures within an Emergency Setting
Keywords:
Battlefield Acupuncture, Distal Radius Fracture, Acute Pain Management, Edema ResolutionAbstract
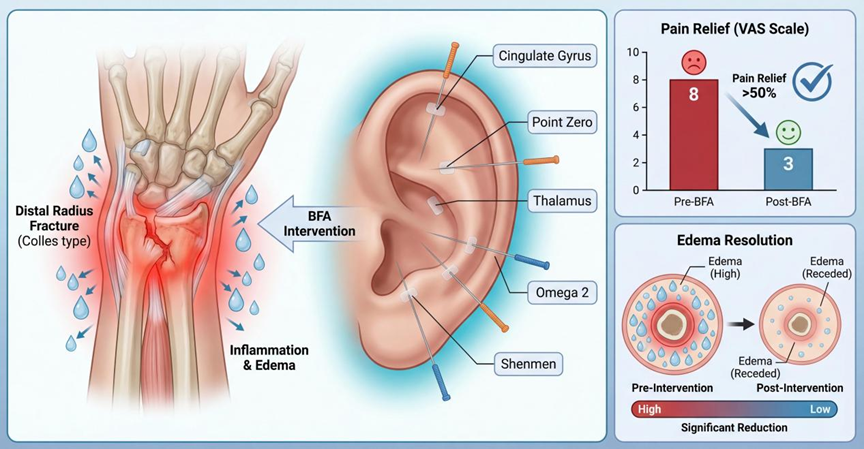
Distal radius fractures (DRF) are highly prevalent traumatic injuries often complicated by severe acute pain and prolonged edema, which hinder early functional recovery and increase healthcare burdens. This prospective, randomized controlled trial evaluated the efficacy of Battlefield Acupuncture (BFA) as an adjunct therapy for 64 patients with DRF during the acute edema phase. Participants were randomly assigned to either a BFA group (n=32), receiving auricular press needles at five specific points combined with standard manual reduction and splinting, or a Control group (n=32) receiving standard care alone. Results demonstrated that the BFA group achieved a superior analgesic effect, with Visual Analogue Scale (VAS) scores decreasing by over 50% within 72 hours post-intervention. Additionally, the BFA group showed significantly faster edema resolution, with the swelling index decreasing by 35.0 ± 4.2% within 72 hours (P=0.003), accompanied by a marked increase in serum β-endorphin levels (+42.3 ± 5.8 pg/mL, P<0.01) and reduced Substance P. No severe adverse events were observed, and the BFA group reported higher patient satisfaction and optimized medical resource utilization. In conclusion, BFA is a safe, effective, and economically feasible intervention that enhances acute symptom control and the early recovery trajectory of patients with distal radius fractures.
References
Alpsoy, A. İ., Güner, S., Kurt, V., & Tekin, S. B. (2025). Can CT Bone Density Predict Fracture Healing? Clinical and Radiological Correlation of Hounsfield Units in Distal Radius Fractures. Bratislava Medical Journal, 126(11), 3091-3096.
Brunken, F., Bullert, B., Grützner, P. A., Vetter, S. Y., & Beisemann, N. (2025). Comparison of 2D and 3D fluoroscopy for intraoperative detection of intra-articular incongruities in distal radius fractures. Journal of Orthopaedic Surgery and Research, 20(1), 824.
Clark, S. P., Ilsø, M., Werlinrud, J. C., Rasmussen, B. S., & Jensen, J. (2025). Distal radius fracture–Supination underestimates dorsal tilt in distal radius fracture radiographs: a case report. Emergency Radiology, 32(4), 663-668.
Diepold, J., Filipp, S., Dussing, F., Steiner, G., Deininger, C., Gotterbarm, T., & Wichlas, F. (2025). Poor fracture alignment equals poor outcome? Analysis of conservatively managed distal radius fractures. Archives of Orthopaedic and Trauma Surgery, 145(1), 442.
Dissaneewate, P., Thanavirun, P., Tangjaroenpaisan, Y., & Dissaneewate, K. (2025). External validation and revision of the Lafontaine criteria for unstable distal radius fractures: a retrospective study. Journal of Orthopaedic Surgery and Research, 20(1), 146.
Hancock, D. W., Barrett-Lee, J. J. T., Abdellatif, A. M. A., White, S., Liu, P., & Roberts, D. (2025). Metaphyseal distal radius fractures in adolescents: is closed reduction and casting sufficient for most?. European Journal of Orthopaedic Surgery & Traumatology, 35(1), 64.
Naito, K., Imazu, N., Ishi, S., Yamamoto, Y., Suzuki, T., Kawamura, K., ... & Ishijima, M. (2025). Central sensitization inventory score after surgical treatment for distal radius fractures. European Journal of Orthopaedic Surgery & Traumatology, 35(1), 187.
Pradyumna, K. Y., Jain, D. K. A., Reddy, R. S., & Fabbro, G. D. (2026). Minimally Invasive Plate Osteosynthesis for Distal Radius Fractures: A Safe Technique with Reliable Clinical, Radiological, Functional and Cosmetic Outcomes. Indian Journal of Orthopaedics, 1-10.
Scioscia, J., Fiedler, B., Ghilzai, U., Birhiray, D., Hauck, J., Chilukuri, S., ... & Deveza, L. (2026). Novel artificial intelligence model predicts the need for reduction of distal radius fractures. European Journal of Orthopaedic Surgery & Traumatology, 36(1), 31.
van Veelen, N. M., Horvat, M., Link, B. C., van de Wall, B. J., & Beeres, F. J. (2025). Locking pegs versus locking screws in volar plating of distal radius fractures: NM Van Veelen et al. European Journal of Trauma and Emergency Surgery, 51(1), 217.
Whelehan, S. P., McCabe, F. J., Merghani, K., Sheehan, E., & Feeley, I. (2026). Assessing the frequency and utility of orthopaedic outpatient department (OPD) attendances of surgically managed distal radius and ankle fractures. Irish Journal of Medical Science (1971-), 195(1), 319-325.
Zhang, C., & Liu, L. (2025). Machine learning prediction model for medical environment comfort based on SHAP and LIME interpretability analysis. Scientific Reports, 15(1), 39269.Shen, Z., Wang, R., Wang, L., Lu, W., & Wang, W. (2025). Application Research on General Technology for Safety Appraisal of Existing Buildings Based on Unmanned Aerial Vehicles and Stair-Climbing Robots. Buildings, 15(22), 4145.